Over one billion people between the ages of 30 and 60 are living with sleep apnea worldwide. It is one of the most common sleep disorders that people experience alongside Insomnia and Restless Leg Syndrome.
Sleep apnea describes a type of sleep-disordered breathing that is caused by an obstruction in the airway, the brain not stimulating the muscles required for breathing during sleep, or a combination of the two. There are several devices and methods for treating sleep apnea, most of which will require a prescription.
A Continuous Positive Airway Pressure (CPAP) device is considered the gold standard for treatment. Outside of a CPAP machine, the best devices for sleep apnea are APAP machines, Oral Appliances, EPAP valves, and implanted muscle stimulation devices. Each device has its own pros, cons, and considerations to make, which we’ll explore in more detail below.
The best device for treating your sleep apnea should ultimately be decided with the help of your healthcare provider, as treatment will vary depending on the type of sleep apnea you experience and other health conditions you may exhibit. Keep reading to learn about the different types of sleep apnea and the best devices for treating it.
The Three Types of Sleep Apnea
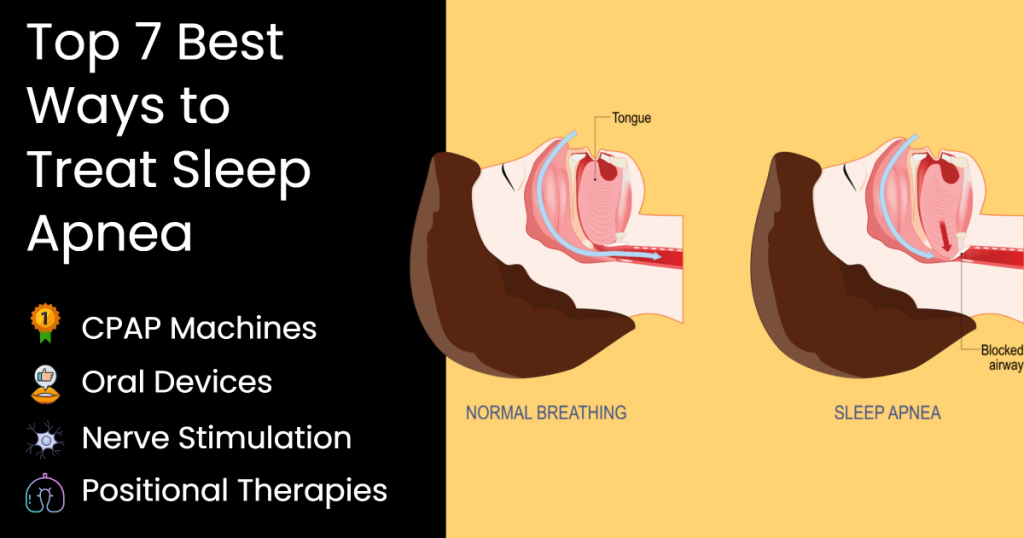
Sleep apnea is a health condition where regular inhaling and exhaling while asleep don’t occur. A person with sleep apnea may take long pauses before inhaling or exhaling during sleep, and it’s common for them to wake up gasping for air or choking.
The three types of sleep apnea are:
- Obstructive Sleep Apnea (OSA): This is the most common form of sleep apnea. Most children and adults with Sleep Apnea have Obstructive sleep apnea, which is caused by an airway obstruction, usually due to excessive tissue in the soft palate. Those who have not had their tonsils removed may also experience OSA more frequently.
- Central Sleep Apnea (CSA): This type of sleep apnea is not common. The problem arises from the brain’s inability to control regular breathing. People with CSA typically need more advanced treatment options that can initiate breathing such as an AVAPS BiPAP Machine.
- Complex Sleep Apnea (CompSAS): Complex sleep apnea is a combination of OSA and CSA and is poorly understood. People with CompSAS are typically diagnosed when they begin treating OSA with a CPAP, only to find it ineffective. This is the most challenging form of sleep apnea to diagnose and treat. It’s common for doctors to explore a combination of therapies, including prescription drugs and advanced BiPAP machines, to treat CompSAS.
The best over-the-counter sleep apnea devices are ideal for mild breathing and snoring issues and aren’t rated to treat sleep apnea. In fact, only products marketed as anti-snoring devices may be sold over the counter, so it’s in your best interest to get a prescription solution that’s FDA-approved and clinically proven to treat sleep apnea, such as the MyTAP Oral Appliance. Snoring and OSA are not the same thing, and relying on an anti-snoring device to treat your Obstructive Sleep Apnea is unlikely to bring you noticeable relief from your sleep apnea symptoms.
7 Sleep Apnea Devices and Therapies That Work
Without effective treatment, sleep apnea can bring your life to a grinding halt. Untreated sleep apnea raises your risk level of Cardiovascular Disease, Stroke, Alzheimer’s, Type II Diabetes, and more. Below is a list of the best devices for sleep apnea, ranging from the most to least effective.
1. CPAP Machine
As stated earlier, CPAP stands for Continuous Positive Airway Pressure. A CPAP device supplies and maintains the same pressure during inhalation and exhalation to hold your airway open during sleep, allowing you to breathe properly.
CPAP machines are roughly the size of a lunchbox or small stereo and use a tube, typically six feet long, to supply air to a mask. CPAP masks come in many styles, but typically supply air to the nose, mouth, or both. Many modern CPAP machines feature a built-in humidifier to help make the constant pressure more tolerable by preventing the airway from drying out. Virtually all CPAP machines have an adjustable pressure relief feature that reduces the incoming air pressure when exhaling for a more natural breathing experience. They also typically have other comfort features designed to make the experience more approachable to encourage continued use.
While there is typically an adjustment period when starting CPAP therapy, those who successfully adapt to CPAP therapy often find the benefits greatly outweigh the drawbacks and wake up feeling refreshed and energized for the day.
Pros:
- Gold Standard for Treating Obstructive Sleep Apnea
- Loaded With Comfort Features to Make Your Therapy More Approachable
- Wake Up Feeling Refreshed and Alert
- Typically Pairs With an App for Tracking Progress and Sleep Data
- Are Available as Travel-Sized Machines
Cons:
- Can be Expensive Up Front and Requires Constant Upkeep/New Supplies
- Adjusting to CPAP is a Lifestyle Commitment
- Managing CPAP Side Effects Like Dry, Itchy Eyes and Mask Soreness
- Tolerating Continuous Pressure is Difficult for Some People
If you’re someone who can’t tolerate the consistent pressure of a CPAP machine, an APAP machine automatically adjusts to your needs and delivers the best pressure for you on a breath-by-breath basis, making for a more comfortable experience overall.
Related Reading: Best CPAP and APAP Machines of 2024
2. APAP Machine
APAP machines are just as effective as CPAP machines in treating OSA but provide the lowest possible pressure needed to hold open your airway instead of providing a set, constant pressure. Most CPAP machines are also available as APAP machines at an increased price, but CPAP and APAP machines will have virtually the same requirements in terms of equipment needed (mask and tubing) and regular cleaning and maintenance.
The advantage of an APAP over a CPAP is that APAPs adapt to your needs and lifestyle changes. In contrast, a CPAP would need recalibration with a new prescription for any significant changes to your breathing based on lifestyle changes you’ve made. With an APAP, you’re merely prescribed a pressure range that typically correlates with the pressure range of the device, allowing it to meet your exact needs for a more personalized therapy experience.
Whether you’re not feeling your best or you’ve made lifestyle changes that enable you to be treated with a lower pressure, an APAP machine will automatically adjust to where you’re at, saving you from unwanted doctor’s visits and more titration studies.
Best for:
- Those Who Can’t Tolerate Continuous Positive Airway Pressure
- Those With Allergies or Who Often Exhibit Cold and Flu-Like Symptoms
Pros:
- Adjusts to Your Needs on a Breath by Breath Basis
- Just as Effective as CPAP
- More Comfortable Than CPAP on Average
- Are Available as Travel-Sized Machines
Cons:
- Typically More Expensive Than a CPAP Machine
- Shares Most of the Same Drawbacks as CPAP
If you’re experiencing Central or Complex Sleep Apnea, you’ll likely be prescribed a BiPAP machine instead of a CPAP or APAP. BiPAP machines are also commonly prescribed for other breathing disorders like COPD.
3. BiPAP Machine
A BiPAP machine is a two-way or bi-level positive airway pressure machine. BiPAP machines use the same tubing and masks as CPAP and APAP machines but have two distinct pressure settings: one for inhaling (Inhalation Positive Airway Pressure-IPAP) and one for exhaling (Exhalation Positive Airway Pressure-EPAP).
BiPAP machines are typically prescribed for more complicated breathing disorders that require a significant difference between inhalation and exhalation pressures or for those that require a higher pressure in general. BiPAP machines have the same minimum pressure setting as CPAP and APAP devices at 4 cmH2O but can reach a maximum pressure of 25 cmH2O, a full 5 cmH2O higher than the maximum pressure of CPAP and APAP machines.
Best for:
- People Diagnosed With a Neurological Condition That Disrupts Breathing
- People Living With Moderate to Severe Lung Conditions
- People Diagnosed With Obesity Hypoventilation Syndrome
Pros:
- Uses the Same Hose and Mask Styles as APAP and CPAP
- Higher Maximum Pressure Setting
- Uses a Distinct Inhale Pressure and Exhale Pressure
- Shares Many Comfort Features with APAP and CPAP Models
Cons:
- Much More Expensive Than CPAP or APAP
- Shares Many of the Side Effects and Drawbacks of CPAP
4. Oral Appliances
Oral appliances for sleep apnea are an effective alternative that doesn’t require you to tolerate air pressure holding your airway open and typically come in one of two forms:
- Tongue Retaining Device: Also called Tongue Stabilizing Devices (TSD), these shield and contain the tongue with a vacuum seal to keep it from falling back into the airway.
- Mandibular Advancement Device (MAD): Mandibular advancement devices treat sleep apnea by holding the jaw forward in an attempt to keep the tongue and excess tissue from falling into and blocking the airway while asleep.
Oral appliances for sleep apnea cannot be purchased over the counter and require a prescription. Only anti-snoring devices that are not rated to treat sleep apnea are available over the counter.
Best for:
- Those With Mild to Moderate OSA
- Adults Who Have Difficulty Adjusting to CPAP Therapy
- Minors With Obstructive Sleep Apnea
Pros:
- Oral Appliances Effectively Treat Obstructive Sleep Apnea
- Much More Affordable Than CPAP or APAP
- Fewer Lifestyle Changes Required
- Some Can Be Readjusted on the Fly
- Doesn’t Require Electricity
Cons:
- Can Worsen Symptoms When Used Improperly
- Can Be Uncomfortable/Take Some Getting Used To
- May Cause Jaw Soreness/Stiffness
- Only Last for 1-3 Years on Average Before Requiring Replacement
Typically, oral devices should be fitted and replaced by a dentist. They must be attached to your teeth or jaws to work correctly.
5. Hypoglossal Nerve Stimulation
A Hypoglossal Nerve Stimulator (HGNS) is a small device surgically implanted inside your chest to help manage sleep apnea. It aids in decreasing sleep apnea symptoms by electrically stimulating the hypoglossal nerve, which runs from the chest to the tongue and controls muscles that move the tongue forward and back, among others.
The nerve stimulator’s job is to monitor your breathing patterns during sleep. If it detects an irregularity, the Hypoglossal Nerve Stimulation Device signals the nerves that control your chest muscles and tongue to adjust and keep the airway open the whole time you’re asleep.
Best for:
- Those With Moderate to Severe OSA
- Those Who Have Tried CPAP Without Success
- Those Who Cannot Tolerate CPAP Therapy
- Those Whose Main Obstruction Comes From the Tongue Collapsing in the Airway
Pros:
- Turned On/Off Via Remote Control
- Device Automatically Responds When On
- Shown to Be Safe and Effective for Treating OSA
Cons:
- Requires a Minimally Invasive Procedure
- Can be Very Expensive
- Only Works if Your Main Obstruction is Caused by Your Tongue
- Can Become Infected and Require Removal/Replacement (Rare, But Possible)
- Not Recommended if You’re Pregnant or Planning to Become Pregnant
- Battery Will Need Replacement After 11 Years
- $30,000 – $40,000 Before Insurance Including Surgery
Hypoglossal nerve stimulation is ultimately something that should only be considered by those who have not had success with CPAP therapy and experience moderate to severe sleep apnea.
Related Reading: Is Sleep Apnea Surgery Right For You?
6. EPAP Valves
Expiratory Positive Airway Pressure, or EPAP, is initiated using a small device that is inserted into the nostrils. By creating resistance to exhale against, EPAP valves, such as the Bongo Rx, use the natural pressure that builds to hold the airway open between breaths. Unlike CPAP, EPAP does not require a machine, doesn’t supply pressure for you, and only uses the power of your own breath to treat sleep apnea.
Not only is EPAP less likely to induce claustrophobic feelings than CPAP, but it’s also been shown to be an effective solution that is easier to stick with long-term.
Best for:
- Those Who Cannot Tolerate CPAP
- Frequent Travelers
- Those With Limited Access to Electricity
- Those With Mild to Moderate OSA
Pros:
- Affordable
- No Electricity Required
- Highly Portable
- Better Compliance Than CPAP
Cons:
- Doesn’t Work for Everyone
- Not Ideal for Moderate to Severe OSA
- Not as Effective as CPAP
7. Position Pillows/Positional Therapy
Positional therapy for sleep apnea employs different devices to keep you from turning on your back during sleep, as moderate sleep apnea symptoms can often be addressed by simply changing your sleeping position. Many people actually experience Positional Obstructive Sleep Apnea that can be moderately addressed with positional therapy techniques, though they aren’t as effective as CPAP for consistently treating sleep apnea symptoms.
Positional therapy techniques often improvise items such as tennis balls, specialized alarms that ring when you roll over, and special pillows to promote side sleeping.
Positional therapy pillows come in different shapes and sizes, including:
- CPAP Pillows: These specially designed pillows are perfect for those already using CPAP machines. A CPAP pillow supports different sleeping positions by using divots and cutouts to more naturally accommodate your CPAP equipment and reduce mask tugging.
- Wedge Pillow: Wedge pillows elevate your lower body from the waist up, helping to relieve some of the gravitational pressure placed on the airway when lying flat on your back. They can also be helpful for alleviating Acid Reflux and GERD symptoms.
- Side Sleeping Pillow: A good full-body pillow like the Medcline Therapeutic Body Pillow can be helpful for positioning the body in a way that helps to prevent your tongue from collapsing into your airway.
Best for:
- Back Sleepers Who Experience Mild to Moderate OSA
- Those Who Experience Positional OSA
- Those on a Budget
- Those Who Are Not Eligible for Invasive Therapies Like Hypoglossal Nerve Stimulation
Pros:
- Many Positional Pillows Offer Multiple Configurations and Are Somewhat Customizable
- Inexpensive and Can Benefit Your Skeletal Alignment, Too
- Some Also Ease Acid Reflux and GERD Symptoms
- Non-Committal Treatment Option
- Can Be Combined With CPAP Therapy
Cons:
- Not As Effective as CPAP
- Not Guaranteed to Bring Relief
- Doesn’t Treat Those Whose Airway is Blocked by Excessive Tissue
Positional pillows can also be combined with other treatment devices like a CPAP machine for maximum results.
Best Devices for Sleep Apnea: Factors to Consider
With various sleep apnea treatment options available, it’s hard to figure out what works and what doesn’t for each specific case of sleep apnea. So, to help you decide, here are four important considerations you should keep in mind in your quest to find the best device for treating your sleep apnea:
Type of Sleep Apnea and Doctor’s Recommendations
Some devices work better for one type of sleep apnea than the other. It’s imperative to consult a sleep specialist and undergo a sleep study to determine which device is ideal for your case. Speaking to your primary care provider about your sleep health and concerns is also a great place to start if you haven’t already been diagnosed with sleep apnea.
Health Insurance
The majority of health insurance policies will cover sleep apnea treatment expenses, but as always, when dealing with insurance, be sure to ask clear questions and get clear answers about exactly what is covered and what you’ll be responsible for. Your insurance policy might favor one treatment over another and may be able to handle more of the cost of a particular type of therapy, so be sure to explore your options with them.
Comfort
CPAP machines yield the best results for people with sleep apnea, but adjusting to CPAP therapy can be difficult. Many people experience claustrophobia at first, and it’s easy to become discouraged and give up on therapy before finding what works best for you. Work with your healthcare provider to explore different mask options and comfort features your CPAP machine may offer to drastically improve your results. If you feel that you’ve tried it all when it comes to CPAP, an oral appliance or hypoglossal nerve stimulator may offer greater comfort.
Re-Evaluation is Always Necessary
If your sleep apnea treatment isn’t working for you or is causing you discomfort, bring it up with your healthcare provider. Some therapies just aren’t made for everyone, and while we always advocate for trying what you can to make things better, sometimes it’s time to throw in the towel and explore options with different therapies instead. While the financial burden can be difficult to bear when something doesn’t work for you, your health and long-term happiness are more important, and investing energy in finding the best treatment for what you need pays for itself in increased energy levels and reduced risk levels for the various conditions and diseases associated with untreated sleep apnea.
Frequently Asked Questions About Sleep Apnea Treatment Devices
What Is the Best Device for Sleep Apnea?
The best device for sleep apnea is a CPAP machine, which provides Continuous Positive Airway Pressure to hold the airway open, allowing you to breathe without obstruction. Oral appliances are a great alternative for those who cannot tolerate CPAP.
What Types of Sleep Apnea Devices Are There?
CPAP/APAP/BiPAP machines, oral appliances, EPAP masks, positional therapy pillows, and hypoglossal nerve stimulators are some of the most popular and effective devices for treating sleep apnea.
What Is the Latest Technology for Sleep Apnea?
Upper Airway Stimulation is the newest solution for those with sleep apnea. UAS devices treat sleep apnea by stimulating the muscles that control the tongue to keep it from collapsing into the airway and are implanted via a minimally invasive procedure.
Which Is Better, CPAP or Oral Appliance?
CPAP is the gold standard for treating sleep apnea, but oral appliances are becoming more popular and can be as effective as CPAP for some people. Consult with your healthcare provider to decide which is better for you.
How Much Does an Oral Appliance for Sleep Apnea Cost?
Oral appliances rated to treat sleep apnea typically cost between $1,500 and $2,000 including dental visits for fitting. Over-the-counter anti-snoring devices can be found for under $200, but they are not rated or recommended for treating sleep apnea.
Can a Pillow Help With Sleep Apnea?
For those who experience Positional Obstructive Sleep Apnea (POSA) which only occurs in certain sleeping positions, a pillow that promotes side sleeping can help ease sleep apnea symptoms.
Can Sleep Apnea Be Cured Naturally?
Mild sleep apnea symptoms may be naturally addressed over time through lifestyle changes such as losing weight, switching sleep positions, quitting alcohol, using decongestants, and getting regular exercise. However, sleep apnea should be medically addressed if you want a lasting solution.
Can Anti-Snoring Products Treat Sleep Apnea?
While anti-snoring products may bring slight relief for people with mild sleep Apnea, they won’t be of much use if you have moderate to severe sleep apnea. In fact, anti-snoring mouthguards can actually worsen moderate to severe obstructive sleep apnea when used improperly.
Bottom Line
A good night’s rest impacts every area of your life by giving you increased energy levels and more mental bandwidth to learn new things and complete tasks required of you by daily life. Sleep apnea is a treatable condition that affects millions of people around the world and devices for treating it are becoming more and more accessible.
CPAP machines, hypoglossal nerve stimulators, mouth devices, positional therapy, and positional therapy pillows are the best devices for treating sleep apnea. Still, you’ll want to consult your healthcare provider to determine the best option for your unique needs.
A home sleep test is the easiest way to start your journey to acquiring a CPAP machine or other treatment device. Ordering a home sleep study is a great and inexpensive first step to ruling out or being diagnosed with obstructive sleep apnea.



