💡 Key Takeaways
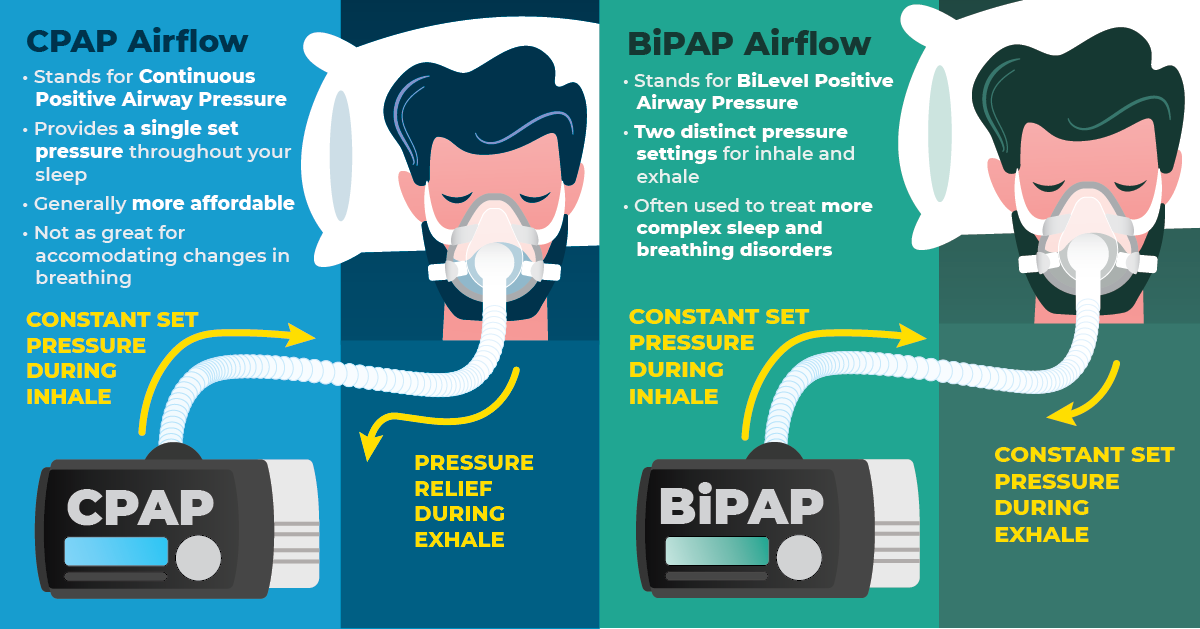
- Two Pressure Levels vs. One: BiPAP offers two different levels of air pressure for inhalation and exhalation, while CPAP provides a constant air pressure throughout.
- Suitability for Conditions: BiPAP is often prescribed for more severe cases of sleep apnea and other more complex respiratory conditions, whereas CPAP is generally the first choice for treating Obstructive Sleep Apnea.
- Ease of Breathing: BiPAP machines make it easier to exhale against the air pressure, offering a more comfortable experience for some.
- Cost Considerations: BiPAP machines are generally more expensive than CPAP machines.
- Complexity and Ease of Use: BiPAP machines may include more advanced features, which might make it more difficult to understand sleep data and machine settings.
Whether you have sleep apnea or suspect you may have it, you are probably familiar with Continuous Positive Airway Pressure Therapy. CPAP is often the first choice for sleep apnea treatment, but despite its popularity, it doesn’t always work for everyone.
In fact, there are several other forms of Positive Airway Pressure Therapy. And if you’re wondering whether one of these alternatives could work better for you, you aren’t alone. That’s why we want to help you understand the differences between CPAP and another method of respiratory support called Bi-level Positive Airway Pressure. So today, we’re discussing BiPAP vs CPAP!
As its name suggests, BiPAP produces two different levels of air pressure, depending on whether you’re inhaling or exhaling. On the other hand, CPAP machines only deliver a stream of air that is set to one specific amount of air pressure. There are also a few other differences between these two devices, which we’ll cover in a moment.
We hope this article gives you a better understanding of not just what a BiPAP machine is and what it does but also whether it would be a good fit for your own needs compared to a standard CPAP device. Let’s get started!
What Is the Difference Between BiPAP vs. CPAP?
The biggest difference between BiPAP and CPAP is in the air pressure being delivered by the machine. CPAP provides air at one constant air pressure setting the entire time, while BiPAP has one pressure level for inhalation and a second, lower pressure level for exhalation.
When starting CPAP therapy, some people struggle to adjust to the feeling of exhaling while air is being pushed into their lungs. With BiPAP, that reduced air pressure setting usually makes it easier to breathe.
What Is a BiPAP Machine?
A BiPAP device is programmed to produce two different levels of air pressure, one for inhaling and one for exhaling. These settings are usually referred to as “Inspiratory Positive Airway Pressure” (IPAP) and “Expiratory Positive Airway Pressure” (EPAP). In most cases, the air pressure used during BiPAP therapy is increased during inhalation, and it decreases when it is time to exhale.
The purpose of having two separate air pressure settings is to make it easier to breathe while undergoing Positive Airway Pressure (PAP) Therapy. This may sound like BiPAP therapy is the obvious better choice for sleep apnea treatment, but most people are able to able to breathe just fine with their CPAP machine, so they don’t actually need bi-level respiratory support.
Related Reading: Best BiPAP Machines Reviewed – Our Top Picks!
What is CPAP Machine?
A CPAP machine delivers a continuous flow of pressurized air to the person wearing the device. This pressure setting is constant, and it is set by your healthcare provider or sleep specialist. It cannot be changed without approval from your provider. Some manufacturers offer products that make it easier to exhale with CPAP therapy, such as the V-Com. However, none of these products are able to actually change the device’s pressure setting.
Is CPAP or BiPAP Better for Sleep Apnea?
When it comes to Positive Airway Pressure Therapy, it’s not a matter of which therapy is best. It’s a matter of which one is right for you. Although most people with sleep apnea use CPAP based on the recommendation of their sleep specialist, there are certain circumstances where a BiPAP might be a better option.
If you are comparing CPAP vs BiPAP to treat your sleep apnea, here are some factors to consider!
- Type of Sleep Apnea: CPAP is typically used to treat most cases of Obstructive Sleep Apnea and may be prescribed to people with mild Central Sleep Apnea (CSA). BiPAP is more likely to be suggested for those with CSA and other serious breathing conditions.
- Portability: There is no ultra-portable BiPAP machine, while there are portable travel CPAP machines.
- Air Pressure: BiPAP machines feature air pressures that go up to 25 cm of H2O, while CPAP stops at 20.
- Cost: CPAP devices tend to be more cost-effective as it is usually cheaper to purchase out of pocket and easier to get approval through insurance.
- Easy to Use: BiPAP machines are usually more complex compared to CPAP. Therefore, a CPAP machine may be easier to use for those who struggle with technology.
- Availability: Because they are so popular, CPAP machines are definitely easier to find, and there are more diverse options and unique features to choose from.
What Are the Indications For When to Use BiPAP Instead of CPAP?
CPAP therapy is usually highly effective for most people with sleep apnea, but how do you know if you need BiPAP therapy? Your doctor will tell you which form of treatment is best based on your overall health and wellness.
Below are some reasons why your healthcare provider may suggest BiPAP therapy!
- Central Sleep Apnea: People who have CSA are unable to regulate their breathing when they are asleep. Because of this, they often need additional support to maintain a normal breathing pattern. While CPAP works for people with mild CSA, it usually isn’t enough for those with more severe cases.
- Complex Sleep Apnea: Much of what can be said about treating Central Sleep Apnea also applies to Complex Sleep Apnea (CompSA). Sometimes referred to as Treatment-Emergent Sleep Apea, this third form of sleep apnea arises when a person with OSA develops CSA after starting CPAP therapy. People with CompSA may respond better to BiPAP therapy when CPAP proves to be ineffective.
- High-Pressure Airflow: Most BiPAP machines can produce air pressures as high as 25 cm of H2O, whereas the majority of CPAP machines max out at 20 cm of H2O. With CPAP therapy, it can be especially difficult to exhale when your pressure settings are so high, So, if you have a condition that requires high-pressure airflow, you are most likely a good candidate for BiPAP.
- Obesity Hypoventilation Syndrome: This form of sleep-disordered breathing is commonly found in people who are very obese and, as a result, breathe too shallowly or slowly during sleep. These breathing changes can lead to respiratory depression, which causes low oxygen and high amounts of carbon dioxide in the bloodstream. If left untreated, this condition has been associated with heart and/or respiratory failure. However, BiPAP is considered an effective treatment method for OHS.
- COPD/Overlap Syndrome: Overlap syndrome is a term referred to when someone has sleep apnea as well as COPD. COPD prevents your body from balancing the oxygen and carbon dioxide in your bloodstream. Overlap syndrome leads to a number of potentially serious health complications, but these complications can be minimized by sleeping with a BiPAP machine.
- CPAP Intolerance: If you cannot tolerate a CPAP machine, BiPAP is an excellent CPAP alternative. Keep in mind that BiPAP is traditionally more expensive than CPAP. So if you want your insurance to cover your BiPAP machine, you may need to clearly document your struggles adjusting to CPAP therapy.
- A Need for Increased Ventilation: If you have lung disease or any other condition that makes it difficult to maintain a normal breathing pattern without respiratory support, BiPAP may be the better choice for you.
Benefits of BiPAP Therapy Compared to CPAP Therapy
Let’s talk about some of the benefits and advantages of using a BiPAP to treat sleep apnea!
- Helps Regulate Oxygen and Carbon Dioxide: BiPAP helps you maintain safe levels of oxygen and carbon dioxide, especially if you have respiratory disease.
- Makes Exhaling Much Easier: BiPAP makes exhaling much easier, even with high-pressure airflow. This makes it easier to adjust to compared CPAP therapy.
- Reduces Risk of Aerophagia: Because CPAP machines can be difficult to breathe out against, they have an increased risk of causing you to swallow air while you are using your machine. BiPAP machines are much less likely to cause this unpleasant side effect, as it is much easier to exhale while undergoing BiPAP therapy.
- Maintains Normal Breathing Patterns: Some BiPAP machines allow you to pre-set your preferred breathing pattern, which can help you maintain normal breathing despite Central Sleep Apnea or other similar conditions.
- Treats a Wide Range of Breathing Conditions: BiPAP machines can be used to treat a wider variety of conditions. So if your condition worsens, you don’t have to go through the hassle of changing your device.
Downsides of BiPAP Therapy Compared to CPAP Therapy
Despite the pros, there are a couple of downsides to using a BiPAP machine in place of CPAP.
- BiPAP Costs More Than CPAP: A BiPAP will cost more than a CPAP. On average, they can cost anywhere from two to four times as much. If you can get your BiPAP covered by insurance, the cost may be reduced, but you may have trouble getting insurance coverage with CPAP being so much cheaper and widely available.
- BiPAP Also Requires an Adjustment Period: Like a CPAP machine, getting used to sleeping with a BiPAP machine may take some time. Although the mask and tubing will feel the same as using a CPAP, those who require very high pressure settings may still struggle to adapt.
Frequently Asked Questions About BiPAP vs. CPAP
What Are the Similarities Between CPAP and BiPAP?
BiPAP and CPAP machines are two different types of non-invasive respiratory support, which both fall under the category of Positive Airway Pressure Therapy. This means that they both deliver pressurized air into the airway, which helps to treat sleep apnea and other breathing disorders.
Why Are BiPAP Machines More Expensive Than CPAP Machines?
If you are looking to buy a BiPAP machine, you will quickly notice how much more expensive they are compared to CPAP and APAP machines. BiPAP machines are complex and have more parts and features compared to CPAP and APAP machines.
Are CPAP and BiPAP Masks the Same?
While some masks may be better suited for someone on BiPAP, most, if not all, CPAP masks will work with a BiPAP machine. However, if your air pressure prescription is for more than 20 cm of H2O, you may need to purchase a specialty mask that will maintain a seal at such high pressures.
Which BiPAP Machine Is Currently the Most Popular On the Market?
There are many different BiPAP devices to choose from, and it’s difficult to say which particular machine is most popular. That said, our favorite BiPAP machine is the AirCurve 10 VAuto BiLevel Machine with HumidAir. Check out our review of the AirCurve 10 and other popular BiPAP machines here!
What Are the Different Types of BiPAP Machines?
There are several types of BiLevel Positive Airway Pressure machines available. Some of the most common include:
- Fixed Pressure BiPAP: The pressure settings for inhalation and exhalation are constant and cannot be changed.
- Auto BiPAP: Allows for automatic adjustments to the air pressure levels based on your breathing patterns.
- BiPAP Spontaneous/Timed: BiPAP ST machines run off of a number of breaths per minute but also allow for spontaneous breathing in between those breaths.
- BiPAP Average Volume Assured Pressure Support: Automatically adjusts the air pressure setting to ensure you breathe in a specific amount of air with each breath.
What Is a VPAP, and Is It the Same as a BiPAP?
The two are very similar, but BiPAP and VPAP are not the same thing. The main difference between VPAP versus BiPAP lies in how the pressures for inhalation and exhalation are selected. Like a BiPAP, the VPAP uses a higher pressure for inhalation and a lower pressure for exhalation. Traditionally, BiPAP machines use pre-programmed pressure settings, while VPAP machines are auto-adjusting.
What Is the Difference Between BiPAP and CPAP and Ventilator?
BiPAP and CPAP machines work by delivering pressurized atmospheric air into your airway. This air pressure may be fixed, as with CPAP. Or it may change based on whether you are inhaling or exhaling, like a BiPAP machine. Ventilators, however, breathe for you, forcing oxygen directly into the lungs and then pushing carbon dioxide out.
Final Thoughts
Continuous Positive Airway Pressure Therapy is often the perfect solution for people with sleep apnea. However, if you have severe Obstructive Sleep Apnea, Central Sleep Apnea or have been diagnosed with other serious respiratory conditions, you may benefit from using a BiLevel Positive Airway Pressure machine. If you have any questions about CPAP or BiPAP therapy, let us know in the comments!




15 Responses
I am very active in sport gym, cycling and power walk. I have suffered with sleep and sleep apnea for a while which has increased my blood pressure during my interrupted sleep evenings. I need to take blood pressure tablets as a result of this.. and causes me not to have a continuous sleep experience. Can you suggest and approach for me? Some this that is compact yet functional.
Hey Ian,
Lots of CPAP users are very active in sports. I am sorry to hear that you are having to deal with high blood pressure and interrupted sleep. I would suggest to you that the most economical option would be a small travel machine and a mask. Another option that you may consider is Provent Therapy. Either way you will need to speak with your doctor because we will require a prescription. If you would like assistance selecting a machine and mask that would best suit your needs we will be happy to assist you if you give us a call at 1-800-356-5221. Here is a link to the Provent Therapy that I mentioned https://www.cpap.com/productpage/provent-therapy-30-day-starter-kit
Whichever option you select please remember that we will require a prescription. We are happy to assist you in obtaining a prescription, just give us a call.
Really nicely written, and informative.
In your article, you don’t say what the letters ST in BiPAP-ST means. I understand that type of machine initiates a breathe for the user, but I’d like to know what ST means.
BTW the machine I’m using now has an APAP mode and also adjustable exhalation relief in both APAP and CPAP mode. I swear my machine, which is not a BiPAP-ST, can initiate a breath on its own. It doesn’t say it has that capability in the user manual. But I think the manufacturer has incorporated the feature without documenting it in the manual. To give the user the best possible experience. This maybe to avoid lawsuits from the legal owners of the ST technology.
Hi Dave,
The ST actually stands for spontaneous timed. Here is some additional information for you found on our FAQ page https://www.cpap.com/cpap-faq/BiPAP-Machine#what-is-the-difference-bipap-and-bipap-st.
Perhaps what you are experiencing is the flow rate of the exhalation relief, or flex feature of your machine (all manufactures call this something different. Eg. Resmed=EPR, Phillips=FLEX, F&P=Senseawake, etc.) Here is some more information on flex technology. https://www.cpap.com/cpap-faq/CPAP-Machine#what-is-c-flex
Is there a “travel size” BiPAP available?
Hi John,
My apologies, but we don’t have any BIPAP machines that are designed specifically for travel however, the Dreamstation BIPAP may be a good option for you. Please see the link below for a look at the Dreamstation Bipap machines.
https://www.cpap.com/cpap-compare-chart-share/2e05
Please let us know if we can be of further assistance. We can be reached at 800-356-5221, or email us at cpap@cpap.com.
Interesting. I wish I’d seen this before I saw my dr. last week. I wonder if I need a Bipap instead of Cpap.
Hey Eileen, it is a possibility. We encourage you to speak with your doctor directly about any concerns that you may have to see if a BIPAP machine would fit you better.
I have a Dreamstation Auto BiPap with settings at 9/13. I had a ruptured brain aneurysm and subarachnoid hemorrhage/stroke in February and they put me on a BiPap machine while I was in the hospital. In the past 2 weeks my AHI has doubled or more from readings of 2 to 4 to 9.3 to 17.6. I don’t know why or what to do about it.
Hi Mary, I would encourage you to speak with your doctor, as they can view your therapy data and make a determination as to if you require a setting adjustment, or what may be causing the increase in your AHI’s.
If you would like to speak with us further, please feel free to contact us at: 1-800-356-5221.
We wish you the best!
I am having differculty @ nite sleeping , a lot of moving in my sleep , sleepy during day , taking naps , I stop breathing even though I am using a c-pap machine, please help me the doc keep saying that my sleep reports look ok , I need help
Hey Rachel, i’m sorry to hear about the troubles with your CPAP therapy. How long have you been using your CPAP machine? The symptoms you are referring to sounds like your therapy isn’t working for you. You may want to suggest to your doctor to increase/adjust your pressure setting.
Also, what type of mask are you using? Have you checked your leak rate? One of the most important factors with successful CPAP therapy, is having a comfortable mask. If you aren’t using a full face mask, you may try switching to one and if you’re currently using a full face mask, you may want to try a different one.
Please be sure to continue speaking with your doctor about the difficulties you are experiencing with your therapy.
Also, please feel free to reach us at: 1-800-356-5221, for further assistance.
Best Wishes!
Hi, If one has complex Apnea, a mix of Central and Obstructive Apnea, can he use a Bipap Biflex without the ST? Without back up rate?
Hi Ricardo, yes you can use a BiPap without the ST. Really, this is something you must speak with your doctor about. The type of machine you get will totally depend on the prescription your doctor writes for you based upon the results from your sleep study.
For further questions, or concerns, please feel free to reach us at: 1-800-356-5221, or e-mail us at: cpap@cpap.com.
Have a great day!